NURSING DEPARTMENT
The Nursing department is the largest department in Lorma Medical Center, compose of 8 in-patient units, 3 Out-Patient Departments and 3 special services like the Audiometry, Laser and the EEG/EMG and 7 special units like the Emergency Room, ICU-Trauma and Stroke Unit, OR/DR/CSR, NICU, Cardiac Catheterization Laboratory, Wound and Ostomy Clinic and the Hemodialysis Units. There are 214 nurses and 48 nurse aides observing the 40 hours a week duty and 1 supervisor to 50 bed capacity.
IN-PATIENT DEPARTMENT

The In-patient department of Lorma Medical Center caters patients who seek diagnostic and therapeutic health care services from the different medical specializations offered by the institution, designed to serve people with health-related concerns required to be admitted for overnight, short term and/or long term care. The department consists of 8 nursing units designed to render holistic and personalized care to patients stratified according to case or condition. Nurse-patient ratio observed is 1:12 and for nurse aid is 1:24.
• 3A station is considered as the OB-Gyn and Surgica Unit as it caters the needs of peri-operative patients. A special Obstetrics and Gynecology room is also found in the unit for women who seek perinatal care where a Breast Feeding room is also included. The unit is made up of 14 air-conditioned private rooms, 4 ward beds for male surgical cases, and 8 for OB Gyne cases. The unit has a total of 26 bed capacity and nurse ratio 1:12.
• Still in the 3rd floor, 3B station is composed of 9 junior suite rooms and 2 big deluxe rooms. The fully air-conditioned junior suite rooms are equipped with their own television unit, watcher’s sofa bed, computer units and refrigerator units. The 2 deluxe rooms are equipped with the above mentioned amenities plus a sala set and a family dining area with microwave oven. These rooms are sometimes used for standard and deluxe executive check-ups. Nonetheless, they can still be used for patients with any case or condition. The unit has a total of 14 bed capacity, nurse ratio 1:12.
• 3C station is a unit where it caters the health care needs of patients with medical conditions and other selected minor surgical cases. A communicable disease (CD) unit is also a part of the station designed for patients who have conditions that necessitate isolation to prevent cross-infection to others. 3C is a 29 bed capacity unit with 5 air-conditioned ward type beds for males, 8 for females, 8 regular air-conditioned private rooms, 6 regular beds for isolation cases, and 2 air-conditioned isolation rooms. It has also 26 bed capacity, nurse ratio 1:12.
• The main pediatric unit is the 3D station as majority of patients less than 18 years of age are admitted in this 32 bed capacity unit. The unit consists of 4 non aircon ward type beds and 19 aircon ward type beds strictly for pediatric patients. For other condition or cases regardless of age, there are also 9 junior executive suites for patient use.
The fourth floor is composed of 3 in patient stations namely 4A, 4B and 4C stations.
• 4A station is much like a medical unit for adults and pediatric patients except for communicable cases, OB-Gyne cases and major surgical patients. Sixteen (16) regular air-conditioned regular private rooms, 3 female air-conditioned ward type rooms and 4 for males make up the unit.
• 4B station or often called as 4th Floor Medical Arts unit, is much like the 3B station. It caters patients of any case from pediatrics to adults in its 12 bed capacity. There are 4 air-conditioned regular private rooms, 6 junior suite rooms and 2 deluxe suite rooms that patients can choose from.
• 4C station is at the 4th floor of the old building. It is a 23 bed capacity unit with 3 air-conditioned male ward beds, 3 for pediatric cases, 2 semi private air-conditioned beds for any case as needed, and 14 junior suite rooms. Patients of any case may be admitted in the unit except for isolation or communicable cases in the ward.
• The last of the in-patient units is 5A station found at the 5th floor annex building. The unit caters all cases both pediatrics and adult except for communicable cases of any kind, perinatal patients and major surgical cases. It consists of 16 regular air-conditioned private rooms, 4 female air-conditioned ward type beds and 3 for males.
The inpatient department is manned by 69 skilled and competent nurses. The ratio of staff nurse and patient is 1:12 respectively. In every unit there is an assigned nurse supervisor to implement an effective and ongoing programs to monitor, evaluate and improve the quality patient care.
EMERGENCY ROOM
The Lorma Emergency Department is a fully fledged department of Lorma Medical Center that has different areas of care which includes the Emergency Medical Services (EMS) or Ambulance Services, Resuscitation Area, Minor Operating Room, Decontamination Area, Birthing Unit, and Observation Unit.
• The Emergency Medical Services (EMS) or Ambulance Services serves as the community’s main access of the hospital if an emergency occurs. The Resuscitation Area is dedicated to patients in need of immediate care such as victims of cardiac arrest. This area has all resuscitative equipment like cardiac monitors, defibrillators, advance airway, intubation and surgical equipment and it is available at arm’s distance including the Emergency Drugs.
• The Minor Operating Room is for procedures like washing, dressing, suturing of wounds, reduction, splinting fractures or dislocations, and other minor procedures. It also has a Decontamination Area for victims of organophosphate poisoning. The Birthing Bed for emergency deliveries. The Observation Unit is for patients who need to be observed for less than 24 hours. Such patients are those with non cardiac chest pain, acute asthma, vague abdominal pain, etc.
• The Lorma ER unit has 9 beds to accommodate patients who will be admitted. It is all equipped with cardiac monitor, pipe-in oxygen and suction machines. The Lorma ER Unit has a triage or triaging system to determine to which pre-designated patient care area the patient should be sent especially in cases such as mass vehicular accident. The Lorma Emergency Department abides on its mission to provide the best quality in emergency care treatment based on holistic personalized health, dedication and Christian concern.
INTENSIVE CARE-TRAUMA & STROKE UNIT

Lorma Medical Center Intensive Care Unit is a 23 – bed facility which caters to critical care in the various areas of nursing such as neurosurgery, cardiovascular, surgical, pediatric and pulmonary. The area consists of 14 private rooms, 4 beds in the ward for adult cases and 3 beds intended for pediatric cases. Critical care nursing is a complex and challenging area of nursing in which nurses use their advance skills to care for patients who are critically ill and needs to be closely monitored.
The rooms in the unit are equipped with cardiac monitors that helps in facilitating comprehensive monitoring of the vital signs of the patients and electrocardiograph tracings to ensure that the patient’s hemodynamic status is stable. The oxygen is placed in the wall unit as well the suction apparatus in each beds in the ICU. There is also a refrigerator where osteorized feeding and medications are stored. The unit also has a storage room where portable cardiac monitor and mechanical ventilators are accessible within their reach.
The unit is a state of the art with high – end facilities which ensures that interventions are done with ease and convenience. As we embrace paperless facility approach, the unit is ready for a more advanced record – keeping. The barcode technique is being practiced in medication administration and vital signs taking.
An ICU Nurse has to be well – trained in nursing techniques and decision – making skills when it comes to taking care of critically ill patients. Before becoming a part of the ICU team, the nurse has to be at least a ward nurse for two years and with exemplary performance in the ward. The nurse will then be oriented by the senior staff in the ICU until the nurse is ready to handle patients. The ICU has various training such as ABG Interpretation, Focus Charting and Documentation as well as the function and responsibilities of bedside and charge nurse are also discussed. The nurses were also trained of Basic Life Support and Advanced Cardiac Life Support and further analysis of ECG is enhanced through ECG Workshop. Selected ICU Nurses has attended training such as 16th Annual Convention Stroke Management: Remembering the Pearls, Avoiding the Perils.
There are also selected staff nurses who are able to join the Intensive Training Program for Nurses at Cardinal Santos Medical Center in San Juan, Metro Manila and the Critical Care Nursing in Philippine Heart Center. Nurses in the ICU are also invited in the Annual Conventions for Stroke Management as well as in Neurosurgery. The nurses are also given the opportunity to have a background on respiratory nursing, pediatric cardiology and kidney transplant. Aside from ICU skills being trained, they are also equipped with soft skills training in leadership and management, ethics in workplace and proper employee relations.
ICU guarantees that the family is in touch with the patient since we welcome family members to be with the patient. With the synergy of other personnel, we make sure that proper care is encouraged.
CARDIOVASCULAR CATHETERIZATION LABORATORY
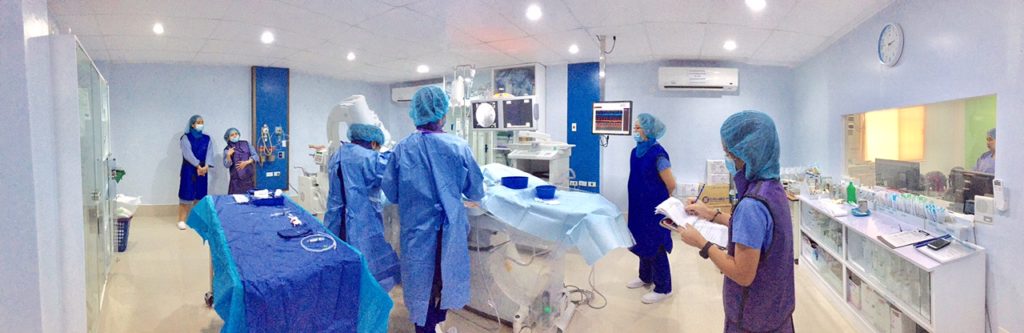
Cardiovascular catheterization is an invasive imaging procedure that allows the interventional cardiologist to evaluate the heart function by inserting small, specialized plastic tubes called catheters into the arteries and veins going to the heart guided by flouroscopy. Cardiac catheterization is used to evaluate or confirm the presence of coronary artery disease, valve disease or disease of the aorta. It also evaluates heart muscle function, heart chambers and measure pressures and hemodynamics of the heart.
It is performed to determine the need for further treatment such as open heart surgery called coronary artery bypass graft surgery. Other than that, Endovascular catheterization is also performed which includes cerebral angiogram, spinal angiogram, renal angiogram, peripheral angiogram to determine blood vessel problems like aneurysm. If aneurysm is determined, endovascular intervention is performed like coiling and embolization.
Other procedures are also performed like pacemaker insertion both single and dual chambers, Implantable cardioverter Device Insertion, Intra-Aortic Balloon pump insertion, Percutaneous Corocary intervention both ballooning and stenting.
The cardiac catheterization lab nurses are registered nurses with a certification under the HB Calleja National Heart Institute with advanced level experience in this discipline. Obviously, cardiac catheterization lab nurses possess a high level of understanding and training in cardiac anatomy and physiology which includes manipulation of specialized and advance machine and equipment like the IABP machine, Physiologic Monitors, Defibrillators, Avoximeters, C-arm machine and hemochron. Most importantly, they are trained to familiarize with all the different types of catheters used for cardiac catheterization in all sizes and use for diagnostic and interventional catheterization.
Prior to the training, Basic Life Support and Advance Cardiac Life Support trainings are necessary. We were trained at the Angeles University Foundation Medical Center in Angeles City, Pampanga and in Mary Mediatrix Medical Center in Lipa City, Batangas from November 9, 2015 to December 18, 2015.
OPERATING ROOM COMPLEX

The operating room complex comprises of four major operating rooms which are all fully equipped to cater different major cases. It also has a minor OR for minor cases and one endoscopy room for endoscopic and colonoscopic procedures. Its labor and delivery room are also equipped to cater the needs of our OB patients.
Here are the breakdown of the number of our rooms inside the OR complex:
- 4 Major Operating Rooms
- 1 minor room
- 1 Endoscopy Room
- 1 Labor room
- 1 Deliver Room
- PACU Unit with 5 bed capaity
- Central Supply Room
The Post Anesthesia Care Unit, which has five beds, caters to our patients who were sedated and are in need of close monitoring after the surgery. Our central supply room is complete enough to supply the different needs of the different OR cases as well as the needs of our patients in the hospital.
The different operations and cases require different fees which all depend in the type of the procedure and its length. The supplies and drugs used are also being charged accordingly.
New Technology/ Innovative provided by the unit: Every year the OR complex seeks for surgical innovations to further compete to the growing market when it comes to health care. We also seek for more new procedures to cater the needs of our patients.Here are some of the innovations that are available in our OR complex.
- Kidney Transplant
- PRP/Stem Cell Therapy
- CVOR
- Laparoscopy
- Fetal/Maternal Monitor
- Hepa Filter
- ERCP
- Colposcolpy
- Neurosurgery
- Plastic surgery
- Phacoemulsification
- Endoscopy, Colonoscopy, Sigmosdoscopy, Bronchoscopy
The OR complex team is composed of 31 Operating Room Nurses, 5 Operating Room Assistants and 7 Operating Room Orderlies and the nurses were trained to respond to different procedures and emergency cases.
Here are the breakdown of the number of OR employees.
Seminars and Training attended for 2016 include the following:
- Fire Safety Evacuation and Response Training.
- Improving Lives Through Science (Endoscopy)
- Wound and Ostomy Care, Saving Lives From Neuro Emergencies
- One Central Sterile Supply Dept. Community:Build! Belong! Branch ORNAP Convention:Expanding the Horizon of Perioperative Nurse.
- Critical Care Course/ Cardiovascular OR.
- Surgical Craniofacial Problem at ER Level and Annual Live Endoscopy Workshop; Image Enhance Endoscopy.
NEONATAL INTENSIVE CARE UNIT / TRANSITION AREA
Lorma Medical Center Neonatal Intensive Care Unit is a 15-bed facility which caters to critically ill infants, premature or sick, needing care in various areas such as cardiovascular, surgical, and pulmonary. The Neonatal Nurses’ care is a holistic approach to the critically ill neonates. Care for the neonates involves management of the health care team and the participation of the mother and/or primary care givers of the patient in preparation for discharge.
The NICU is equipped with an incubator, infant warmers and cardiac monitors that facilitate close monitoring of critical neonates. The oxygen and compressed air sources are mounted on the wall where the suction apparatus can also be connected, when needed. A digital mechanical ventilator is dedicated in the inner NICU.
The unit is conveniently located adjacent to the Operating Room and/or Delivery Room for the Neonatal Nurse’s ease of access when a delivery is inherent. The NICU is just a step away if and when a compromised newborn needs advanced care.
TRANSITION AREA
The Transition Area is an area in the NICU dedicated for the observation of well babies that cannot be roomed-in with their mothers immediately as justified by their Attending Physician.
The infants in this area are closely monitored for untoward signs and symptoms.
MILK BANK
The NICU/ Transition Area has a dedicated Milk Bank which holds donated breastmilk from mothers with sick babies and from lactating employees.
It is being maintained by the Neonatal Nurse keeping record of the donated milk that comes in with proper labels and strictly follows the “First in, First out” Policy.
NICU PERSONNEL
The NICU personnel are well-trained in the Essential Intrapartum and Newborn Care that encompasses the basic skills of a Neonatal Nurse. It all starts when an infant is born where care is immediately given. From the mother’s womb, the newborn baby is delivered on to the mother’s abdomen where thermoregulation and assessment are done almost simultaneously to aide in the first breastfeed, whether in Normal Spontaneous Delivery or Caesarian Delivery.
The NICU Nurse must have basic knowledge of asepsis and antisepsis since the patients are in their most sensitive stage of life. They often assist in Umbilical Catheterization which is a more accessible and practical way of starting intravenous fluids in newborns. It is done in the convenience of the NICU with only minimal sterile equipment to prepare.
The Neonatal Nurse in training is shadowed by a seasoned senior in receiving newborns in the Operating/Delivery Room, taking in mind the four simple time-bound steps of the EINC: 1) Immediate and thorough drying of the newborn, 2) Early skin to skin contact between the mother and newborn, 3) Properly timed cord-clamping and cutting, and 4) Non-separation of newborn from mother for early breastfeeding. They are also trained in Lactation Management and Education to better equip them in handling mothers and newborns that have difficulty or reluctance in breastfeeding. A neonatal nurse is also trained to have Intravenous Therapy and ACLS/BLS certification.
The Neonatal Nurses attended the Helping Babies Breathe Program brought to the Philippines last 2015 by the American doctors onboard the USNS Mercy, echoed by Dr. Daisy Evangeline C Garcia. As a second installment to the HBB Program, they attended the Neonatal Resuscitation Program which honed their skills as neonatal nurses.
Newborn screening is an essential part of the NICU where majority if not all, of newborns are subjected to. Neonatal nurses are trained in the collection of samples, to storage, to packaging and to processing for sending to the nearest NBS Center. They also help in communicating back and forth with the mother and the NBS Center for neonates with positive NBS results. Selected nurses are sent to annual NBS Conventions to brush up on the latest NBS innovations in the country.
Lorma Medical Center has been an Exemplary Achievers Awardee since 2007 for the implementation of Newborn Screening as part of an infant’s Newborn Package when delivered at our institution. Lorma offers both the Basic and Expanded Panels of the NBS. The Neonatal Nurses make sure that every newborn delivered in our institution is screened for the panel of disorders, coordinates with the Newborn Screening Center and the child’s parents in dealing with positive results, and arranges for the parents to acquire the results even after discharge.
Lorma Medical Center was accredited as a Mother-Baby Friendly Hospital in 2013 and was reaccredited as such last 2016. The Mother-Baby Friendly Hospital Initiative is a program of the Department of Health fostering the health and wellness of both the mother and child through early breastfeeding. The NICU, under the direct supervision of the Breastfeeding Committee, has been instrumental in the implementation of the Breastfeeding Policy and the Lactation Management training of the employees.
The Neonatal Nurses attend monthly Nursing Service meetings that include a Spiritual Enrichment Seminar. During the course of a year, they also attend trainings for Leadership and Management, Ethics in the Workplace and Proper Employee Relations.
WOUND AND OSTOMY CARE CLINIC
Lorma Medical Center’s Wound and Ostomy Care Clinic is one of the newest facilities of the hospital. It caters to patients with acute and/or chronic wounds, and with different kinds of stoma like colostomy, tracheostomy and the like. This one-bed facility is situated at the Second Floor of the Hospital’s West Wing Building and is within the premises of the Out-Patient Department 3.
The Wound and Ostomy Care Clinic is manned by two staff nurses, who had recently attended trainings and seminars regarding this new field of nursing. These nurses serve in both in-patient and out-patient bases. Procedures done are in connection with the surgical and/or medical doctor’s orders in the patient’s chart. The Wound and Ostomy Care Nurses are guided by the Special Services’ Supervisor, the Nursing Director, and the Medical Director.
Sources of the Wound and Ostomy Care Clinic’s wound dressing and stoma appliance materials mainly come from the hospital’s Central Supply Room. Modern dressings and stoma appliances will still be coordinated and purchased from available distributing companies.
In coordination with The Medical City’s Stoma and Complex Wound Care Clinic’s manager Mr. Rhyan Hitalla, a 2-day Congress and 2-week exposure training were attended by the Lorma Medical Center’s Wound and Ostomy Care Nurses. A 1-day workshop, organized by the Philippine General Hospital, was also attended. Furthermore, since certifications in this field of nursing are obtained outside the Philippines, the Philippine Wound Care Society is now organizing their first Enterostomal Therapy Course to certify more nurses, to expand this nursing career, and to provide quality wound and stoma care in the entire country.
HEMODIALYSIS UNIT
Dialysis is the process of removing waste products and excess water in the body which a normal kidney does. It could be applied to patients with acute and chronic renal problems. A ‘dialyzer’ is used which in layman’s term is referred to as an artificial kidney. Blood passes to and from two mechanisms. An arterial side where blood and waste products are pulled out and a venous side where the clean filtered blood is returned to the body. Creatinine is the confirmatory test for potential dialysis patients. Alongside these are hematocrit, hemoglobin and potassium. Patients are required to have their Hepatitis Profiles (Anti-HCV and Anti-HBsAg) taken before starting treament and every 6 months thereafter to check if they are positive for Hepatitis B and C or in need of a Hepatitis Titer.
Patients who test positive have a separate machine. A patient may opt to have an arteriovenus fistula, arteriovenus graft or permanent catheter created after having a femoral or intrajugular catheter as their temporary access for a month. Currently, there are two machines being used the Fresenius Medical Care 4008s and 5008s. These machines go hand-in-hand with Reverse Osmosis (RO) water, Acid which contains electrolytes and minerals and Bicarbonate all serving to buffer the filtering process. Both cater to suit the needs of each patient and their fistula. Each machine has specific modes to make blood filtering efficient and effective. The blood flow and ultrafiltration (UF) rate are manually inputed following the Nephrologist’s order and the Dialysis Nurse’ assessment. Some patients choose to have their treatments thrice a week which is most recommended. Others, have it twice or once a week.
Furthermore, each patient has a specific heparin regimen so as to prevent clotting regardless of the brand they use. In some instances, heparin-free treatments are given to patients with bleeding following a strict Normal Saline Solution flushing schedule. After every treatment, most patients are injected with Epoietin Alfa. This is due to the fact that their hemoglobin levels are low and below the normal values. Each treatment is started and ended with weight-taking and vital signs monitoring from time to time. Each treatment is started and ended with weight taking,proper assessment, and vital signs monitoring. Patients are expected to reach the target dry weight and be relieved from difficulty of breathing if applicable with stable vital signs and no complaints post treatment.
Dialysis nurses are all Certified Nephrology Nurses who underwent five-week training and met specific requirements to be officially recognized. First, s/he has to be a Bachelor of Science in Nursing (BSN) Graduate and a registered nurse. S/he has to have an Intravenous Therapy (IVT) License, Philippine Nurses Association (PNA) membership, Basic Life Support (BLS) and Advanced Cardiac Life Support (ACLS) Training and a formal training from a Dialysis institution.
S/he should have also completed the Hepatitis Vaccine schedule and should test negative for Hepatitis Screening. Should the individual have inadequate antibodies, a booster shot is a required due to constant exposure. After which s/he should have at least 3 months clinical exposure in a Dialysis Facility or at least 6 months hospital experience. S/he should complete 12 units of renal-related seminars and updates after being a member of the Renal Nurse Association of the Philippines (RENAP). The individual takes the National RENAP examination held at the Heart Center of the Philippines or their other established satellite offices and it is only after passing that s/he can be officially recognized as a Certified Nephrology Nurse.
SPECIAL SERVICES
• LASER
Laser is used to correct refractive errors (i.e. how your eye focuses light) of patient suffering from cataract, diabetic retinopathy and glaucoma because it blocks the entrance of light in the eyes of the patient. The machines to be use are the following:
- Perimetry – measurement of person’s field of vision
- Argon Laser – a laser with ionized argon as the active medium and with a beam in the blue and green visible lightspectrum; use for PHOTOCOAGULATION
- Fundus Camera – is a specialized low power microscope with an attached camera. Its optical design is based on the indirect ophthalmoscope. Fundus camera are described by the angle of view – the optical angle of acceptance of the lens.
The nurse assigned in the unit had training on Flourescein Angiography and Visual Field or Perimetry. In the process of Flourescein Andiography the technician will inject a dye after negative skin test. Confirm adequate papillary dilatation with Tropicamide Phenylephrine. Position patient for photography on the fluorescein andiography machine. Focus on designated field or view. Take initial colors and red free shots of the fundus. Make preparations for IV flourescein dye and insert to the metacarpal vein. Position patient in front of the flourescein andiography machine. Establish internal fixation device. Inject flourescein dye into vein and start concurrent timer. Capture posterior pole photos of both eyes.
Shots are continued for both eyes until mid-phase and late phases. Observe for any untoward signs and symptoms and of allergy. For perimetry, instruct patient to always look straight ahead at the steady yellow light. Other lights will flash one time of to the side. Some light will be bright, some will be bright, some will be dim. Press the button whenever you see one of the lights. You are not expected to see all of them. The test is design so that you may see fewer than half of them. You may blink when you press the button. If you need to rest, hold the button. Do not put pressure on the switch unless you are responding.
• AUDIOMETRY
Audiometry is a test to identify and diagnose hearing loss. This will enable the doctor to diagnose hearing problem to children, adults and elderly. With correct diagnosis of specific pattern or hearing impairment, the right type of therapy will include hearing aids, corrective surgery or speech therapy.
An audiologist is a specialist in detecting hearing loss that uses an audiometer for audiometry testing. Testing of hearing hearing loss is done in a sound proof testing room.
The equipment emits sounds or tones at their various frequencies or pitches at different volumes or level of loudness. On the other hand, the person will undergo testing wears a set of headphones that blocks distracting sounds and delivers the tests tone to one ear at a time. When sound of a tone is emitted, the patient holds up a hand or finger to indicate that sound is detected. Then the audiologist lowers the volume and repeats the sound until the patient can no longer detect it. There is a second type of audiometry testing by using head bands rather than head phones. It is worn with a small plastic rectangle that fit behind the ears to conduct sound through the bones of the skull.
The patient can sense the sound transmitted as vibrations through the bones to the inner ear. The test like head phones that the tones repeated at various frequencies and volumes. The result is recorded on a grid or audiogram. This will enable to give prescription to use hearing aid in case of hearing loss.
The technician had undergone a Pure Tone Air conduction Audiometry Training to specialize in the field of detecting hearing loss thru audiomerty machine.
• ELECTROMYOGRAM (EMG) / ELECTROENCEPHALOGRAM (EEG)
The Electromyogram or EMG is a unit that monitors or detects the muscular activity that can occur in many diseases and conditions which muscular dystrophy, inflammation of muscles, pinched nerves damage which can damage the arms and legs and disc herniation.
The electroencephalography or EEG which is a neurological test by attaching an electrodes on the head of a person to measure and record activity in the brain. The purpose of the EEG is known as the brain wave test to diagnose and manage epilepsy and other seizure disorders. It will assist in the diagnosis of brain damage and diseases such as strokes, tumors, encephalitis, mental retardation and sleep disorders. This will enable the psychiatrist to distinguish conditions such as schizophrenia paranoia and depression cause by degenerative mental disorders such as Alzheimer’s and Parkinson’s diseases.
The technician to specialize the EMG and EEG procedures to avoid errors or mistakes in the diagnosis of the patient and will give also the right tract for the doctor to give an accurate medication.
• OUT- PATIENT DEPARTMENT 1, 2, 3
The outpatient department of Lorma Medical Center caters walk-in patients, sick or well, who seek consultation, medical advices and treatments from the different medical and health-related specializations offered. It is a part of the institution designed to serve outpatients, people with health-related concerns who visit the hospital for treatment, diagnosis, maintenance or follow-up, but are not required to be admitted for overnight to long term care.
• OPD 1 is located at the ground floor of the Lorma Medical Center old building south wing which offers medical disciplines such as internal medicine, pediatrics, cardiology, orthopedics, otolaryngology, pulmonology, dermatology, family medicine, nephrology and transplant, obstetrics, ophthalmology and other specialties.
• OPD 2 is found at the second floor medical arts building. Physicians’ clinics offer a wide range of adult medicine such as neurology, general surgery, cardiology, neurosurgery, urology, dentistry, dermatology, plastic surgery, pulmonology, otolaryngology, gastroenterology, general internal medicine and others.
• OPD 3 is found at the second floor of the Lorma Medical Center old building and is the newest of the three as it opened just last year 2016. The medical clinics here offer services in internal medicine, otonasolarngology, obstetrics, surgery, urology, neurology, pediatrics, rheumatology, endocrinology and pulmonology. Special disciplines are also offered in this area like interventional cardiology, head and neck cancer, gynecologic oncology, surgical oncology, pediatric surgery and adult-pediatric urology,
Clinics at the Outpatient departments have their own opening and closing schedules.
Nurses are at the OPD nursing stations are open from 8 am to 5 pm and extends to 7 pm as necessary.
• THE INFORMATION / ADMITTING DEPARTMENT

The Information/Admitting Department is also under the Nursing Department and is located at the north wing of LORMA Medical Center beside Emergency Room. It is the center of communication of the entire institution. The department has 5 digital telephone units, one fax machine, 2 digital intercoms and 4 analogue intercoms, a centralized paging and sound system.
We have 12 trunk lines and lines for Globe/Smart connected to the telephone system (PABX) which is essential for a faster flow of communication. We also have VONAGE and SKYPE lines catering international calls. There is also one two-way radio which aides in faster relay of messages to orderlies and 2 computer units, one unit at the Information and one at the Admitting specifically used for admission process, with 2 printers. There is also a display monitoring system for a more organized admission process and one cell phone unit used in the admission notification for doctors.
Telephone trunk lines:
888-2616 700-0000 700-0400
888-2617 700-0100 700-0500
888-2618 700-0200 700-0600
888-3448 700-0300 700-0900
Telefax line: 242-3621
Cellphone: 09175972594
Cellphone(PABX connected):
Globe – 09175833069
Smart – 09988686485